Uric acid (UA) is a by-product of our metabolism that is normally excreted through the kidneys. Increased UA levels in the blood can be caused by a persons’ diet (e.g. alcohol intake and purine rich foods), certain diseases (e.g. psoriasis or cancer treatments), or if the body has an impaired ability to excrete UA (e.g. kidney disease).
The abnormally high concentration of uric acid in the blood is called, hyperuricemia. Over time, hyperuricemia slowly causes a gradual accumulation of uric acid deposits throughout the body, particularly in joints and bones but also in other tissues such as the skin and blood vessels.
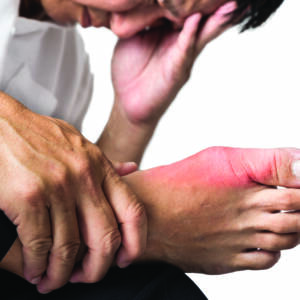
The accumulation of UA, as monosodium urate crystals, in the joints is the basis for gout development. Gout is well known to most and is actually one of the most common forms of arthritis. Gout is a relatively well-understood condition and simple to treat, but nonetheless gout can, if inadequately treated, pose significant management challenges. When left untreated gout becomes chronic and will not only cause joint damage, but can also contribute to the development heart and kidney complications.
Professor Johannes (‘Hans’) Nossent, who holds WA-AOF supported Chair of Rheumatology at UWA and his team at UWA have worked together with the investigators of the Busselton Health Study to study the frequency and risk for cardiovascular disease (CVD) events and/or dying when having high levels of uric acid and/or gout over time.
The results have been presented at the large Annual Scientific Meeting of the European League against Rheumatism (EULAR) held in London in 2016 and have now recently been published in the peer reviewed scientific journal BMC Cardiovascular Disorders (Nossent et al. BMC Cardiovascular Disorders (2016) 16:256, DOI 10.1186/s12872-016-0421-1).
The investigators measured the level of uric acid (normal level under 0.42 mmol/L) amongst 4,173 participants in the 1994/1995 Busselton Health Survey. The majority (84%) did not have CVD at the beginning of the study (healthy group), but 16% of the participants did (CVD group).
The investigators then determined whether and how high levels of uric acid influenced the risk of later cardiovascular events or death in the two groups as evidenced from WA wide hospital discharge and mortality registries during 15 years of follow-up.
Hyperuricemia was present in 9.4% of the healthy participants and in 16.5% of those with a history of CVD, and had also led to gouty arthritis in 1.4 and 3.5% of the groups, respectively. During the fifteen years of observation, heart and blood vessel disease requiring hospital admission occurred in 13% of the health and 43% of the CVD group, while death occurred in 4.5% and 17% respectively.
A statistical model that accounted for a person’s age and gender, found that for each 0.1 mmol/L rise in UA level in the healthy group was associated with significantly increased risk for overall death (19%), cardiovascular death (27%) and new onset of CVD (28%).
When other risk factors for CVD such as smoking, high blood pressure, high cholesterol, being overweight were taken into account as well, the risk associated with uric acid levels decreased to 15%, 17% and 9%, respectively but were no longer statistically significant. The risks associated with rising UA levels in the group with already established CVD were even higher, but again reduced after considering other risk factors.
The investigators concluded that approximately 250,000 West Australians have increased blood levels of uric acid. This is not only associated with manifest gout in 40-50,000 West Australians, but also participates in the complex pathway of metabolic factors that increase the risk for cardiovascular disease.
As dietary and lifestyle factors can reduce uric acid levels, these figures indicate a clear need for wider attention to uric acid levels.
by Prof Johannes Nossent MD, PhD, FRACP, Rheumatology and Musculoskeletal Medicine, UWA
Reference: Nossent, J., Raymond, W., Divitini, M. and Knuiman, M., 2016. Asymptomatic hyperuricemia is not an independent risk factor for cardiovascular events or overall mortality in the general population of the Busselton Health Study. BMC Cardiovascular Disorders, 16(1), pp.1 – 8.